Are you wondering how healthcare, an industry capable of life-saving miracles, has become overwhelmed by financial challenges, inefficiencies, waste, and a loss of public trust? Many experts point to systemic issues rooted in outdated mindsets, bureaucratic battles, and misaligned priorities. If you're a healthcare provider, leader, or decision-maker, understanding how we got here—and, more importantly, how to start turning things around—is essential.
In this post and as discussed in its associated podcast, we'll explore the core reasons behind the current healthcare crisis, from cultural biases to regulatory games, and most critically, how to shift from a reactive, token compliance mindset to a proactive, generative safety culture. By the end, you'll have a clearer idea of practical steps to take your organization from surviving to thriving, with better patient outcomes, happier staff, and a healthier bottom line.
The Roots of the Healthcare Crisis: How Did We Get Here?
Healthcare has achieved astonishing progress over the past 50 years: lifesaving organ transplants, neonatal care, and cutting-edge therapies like those that can successfully treat cancer. Care that once seemed like science fiction but today help people live longer and healthier lives. Yet, paradoxically, the industry is in trouble. Margins are razor-thin, staff burnout is at an all-time high, and rural hospitals face imminent closure, leaving vulnerable populations without access.
Why did this happen? According to Darlene Bainbridge—a seasoned expert with nearly five decades in healthcare quality and leadership—much stems from the industry's historical focus on chasing technology, revenue, and regulatory compliance rather than controlling costs, ensuring meaningful outcomes and protecting the patient/provider relationship. Something Jim Collins describes as the act of “chasing more” while denying the importance of being in control of all the new risks that come with the advancement of patient care.
The Evolution of Quality and Its Impact
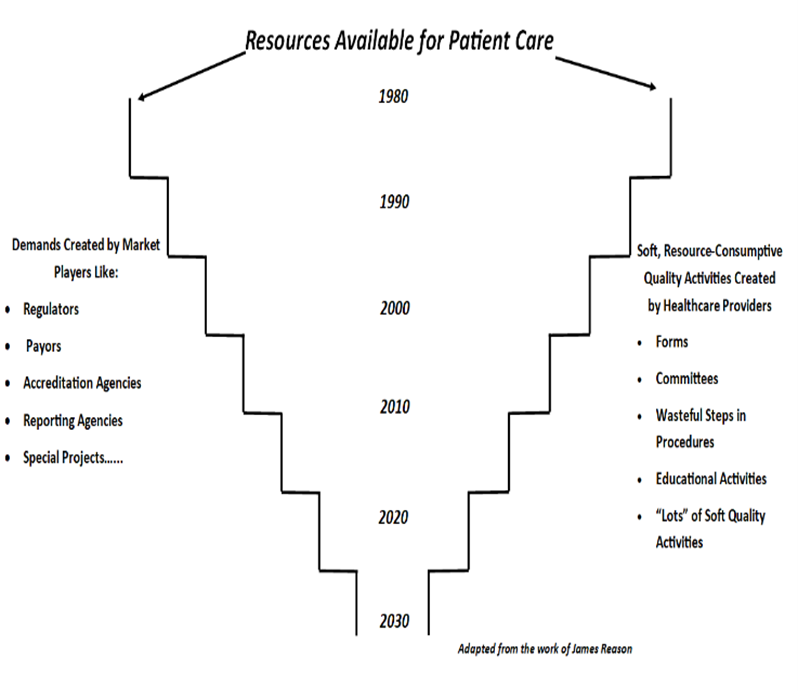
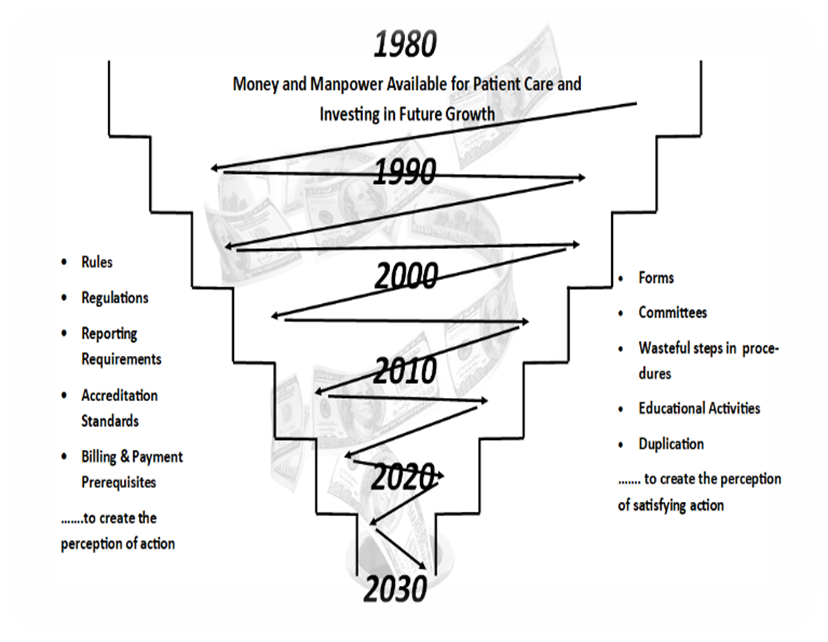
In the early days of healthcare’s technological revolution, quality programs evolved with a focus on assurance driven by outside forces: meeting standards, passing surveys, and ticking boxes. Bainbridge describes how this approach led to a destructive game of "tit for tat”—organizations doing the minimum required to satisfy regulators and surveyors rather than genuinely prioritizing the kind of patient safety and operational control that would lead to long-term success.
She explains that this mindset, rooted in a game of "minimal compliance," has drained resources, fostered distrust, empowered outsiders who once only operated on the periphery of the patient/provider relationship, and discouraged healthcare from managing risks in ways that would protect the power, influence, earning potential, and goodwill that it was positioned to enjoy. It’s like spending so much time filling out forms that you neglect the actual safety of patients.
The Insidious "Game of Tit for Tat"
This behavior, Bainbridge notes, is akin to a poorly played chess game—organizations making moves that are just enough to avoid penalties and immediate consequences but not enough to prevent long-term harm and loss. They react to new standards, implement superficial fixes, and avoid addressing root causes of errors, waste, inefficiency and financial loss. Convincing themselves that with every performative move they are winning when, in all reality, they have been feeding the industry’s slow and insidious story of demise.
She highlights real-world examples: hospitals building expensive new buildings while cutting the very staff that determines profitability, prioritizing regulatory checklists over the actual delivery of error-free care, and focusing on numerical rankings instead of patient outcomes. A reactionary culture that perpetuates waste and erodes trust—causing public confidence to plummet from 85% in the 1960s to about 30% today.
How the Misinterpretation of Quality Drives Waste and Frustration
Quality as a Measure of Minimal Compliance, Not Improvement
Bainbridge emphasizes that in healthcare, like in any other industry, quality should be about controlling everything that could be financially, operationally, or reputationally harmful. Aligning the business needs of the provider with the relationship needs of the buying customer—the American people. Instead, the industry has equated quality with a game of compliance, and more dangerously minimal compliance,—checking boxes rather than proactively managing risks and ensuring public trust.
She traces the evolution through how the industry migrated from "quality assurance" (QA) to "quality improvement" (QI) to "performance improvement" (PI). Unfortunately, too often having hospitals tweak language without changing processes, leading to a false sense of progress. Shuffling language to mask the underlying problem: a culture of reacting to external pressures rather than internally managing risk, safety and costs.
The Impact of the "Tit for Tat" Approach
The "tit for tat" mentality—dating back to the 15th century—is alive and well in healthcare. Hospitals and all types of providers feed an illusion of saving money when they minimally achieve compliance with activities that satisfy influencers like regulators and surveyors. Too often creating a mountain of paperwork, policies, procedures, and activities that don't necessarily improve real safety but consume the money and manpower it takes to be financially, operationally, and reputationally strong.
For example, Bainbridge recounts how hospital survey processes are too frequently satisfied with new forms and checklists that wastefully consume staff time to satisfy compliance measures, not deliver on outcome measures—sometimes tying up as many as five nursing FTEs just to manage a single new form where the outcome is performative adherence, not better patient care! Leading to burnout, staff turnover, and neglect of critical patient care issues.
Waste, Unnecessary Costs, and Lost Opportunities
Healthcare wastes roughly a trillion dollars annually due to redundant processes, unnecessary procedures, misaligned investments and managing to the “100” in the 1:10:100 Rule. Causing hospitals to spend roughly thirty cents of every shrinking dollar they earn on wasteful costs and losses that eat into resources that could be used for patient care, staffing, technology, or patient care innovation.
Bainbridge points out how industry approaches to things like EHR mandates could introduce the kind of breakthrough performance the industry desperately needs but generally do not as spending is dedicated to “chasing more” managed by tools that promote after-the-fact minimal compliance, not transformative advancement. Focused on the illusion that some satisfying action perceived to keep money in the pot for “chasing more” is enough with little consideration for the net loss delivered when all the math is done. Chasing new money in the absence of a business model where money and quality are managed like they are two sides of the same coin—and then compounding size of their losses with the kind of waste and inefficiency that create super tiny margins. Rarely improving financial, operational, and reputational health in the kind of meaningful ways create long-term because of an attitude about quality that escalates costs and frustration.
From Minimal Compliance to a Generative Safety Culture
Reframing Quality: The Control of Risks and Losses
Instead of settling for a game of minimal compliance and all its associated costs, organizations looking to survive need to adopt a generative safety culture, where the goal is to manage risks proactively in business-smart ways—before harm and avoidable losses occur. This involves:
● Empowering staff to identify and report risks without fear
● Eliminating unnecessary costs and bureaucratic layers
● Investing in process improvements that drive efficiency and directly impact outcomes
● Managing to “1” in the 1:10:100 Rule instead of the “100”. Getting it right the first time rather than cleaning up messes
● Prioritizing patient needs over tit for tat
All qualities that Bainbridge prioritized when she was building SQSS (Strategic Quality Support System) to help hospitals manage their ever-growing list of risks and quality demands is ways that save money and free up manpower through efficiency, better risk control, and the elimination of wasteful activities.
Breaking Free from "Tit for Tat" and the "House of Cards"
Healthcare, according to Bainbridge, has become like a fragile house of cards—built on layers of tit for tat, misaligned incentives, and compliance-driven behaviors. A house of cards where providers of care are now positioned as the first to go down—finding little comfort in the fact that they won’t be going alone. Having to decide what they will now do to save themselves from what Jim Collins points out as three potential futures. One where they survive as a preferred provider because they embrace the changes necessary to do so; one where they capitulate to irrelevance in an increasingly competitive environment; or one where, after enough time and enough unprofitable fallacies, they cease to exist. Leaving our hospitals to:
● Recognize that minimal compliance is not enough
● Shift focus from reacting to outside pressures to internally controlling risks in business-smart ways that will lead to patient loyalty
● Align leadership goals with meaningful safety and quality outcomes
● Learn the value of managing money and quality like they are two sides of the same coin
This shift requires leadership commitment, cultural change, and strategic retooling of internal systems, including quality programs, risk management practices, staff training, and data management.
Practical Steps to Start the Transition
● Assess internal culture: Are your staff encouraged to identify risks proactively and prioritize patient needs? Or are they just ticking boxes?
● Streamline processes: Eliminate redundant forms and processes, focus on high-impact activities, and reduce task overload with tools like SQSS.
● Lead from the top: Hospital leadership must set the tone—quality is everyone's responsibility, and it starts at the executive level.
● Prioritize outcomes, not just processes: Measure success with outcomes of patient safety, satisfaction, and operational efficiency-not compliance.
● Adopt a risk-based mindset: When deploying new services or technologies, evaluate potential risks upfront and manage them effectively before they become a problem.
How to Start Fixing Healthcare: Key Takeaways
● Recognize that the current quality model is a result of outdated mindsets rooted in compliance and superficial fixes.
● Shift leadership focuses from passing surveys and checking boxes to controlling risks and delivering on outcomes.
● Use data and tools that promote proactive risk management instead of bureaucratic fatigue.
● Empower staff to take ownership and identify issues before they escalate.
● Invest in process improvements that save money, reduce waste, and improve patient satisfaction.
● Think long-term: move from a reactive, checkbox culture to a generative safety ecosystem where the payoff created by cultural, operational, and strategic change is transformative.
● Adopt empowering systematization: the kind that offers the profound reorganization of systems that shift patient care conditions. behaviors, and power structures in a measurably desirable direction—overcoming the losses associated with status-quo biases.
Final Thoughts
Healthcare's future depends on our ability to change from within—redefining quality as the control of risks, not just paperwork and passing surveys. The key is leadership’s committed to fostering a culture where safety, efficiency, and optimal patient care are ultimately about outcomes, not compliance. By doing so, we will rebuild trust, improve health system resilience, and create a sustainable model for delivering truly excellent care.
Are you ready to lead the change? Start today by evaluating your internal practices, eliminating unnecessary bureaucracy, and empowering your team to make safety the foundation of everything they do.
FAQ: Key Questions About Fixing Healthcare
“Successful people ask better questions, and as a result, they get better answers.”
Tony Robbins
What does "quality" mean in healthcare?
Quality should be about controlling everything that can negatively impact safety, costs, or reputation. It’s about proactive risk management and sustainable control through strong quality activities, not just minimally satisfying standards, passing surveys, filling out forms, and reporting numbers.
How can hospitals move away from a "tit for tat" compliance culture?
By shifting focus from minimally satisfying external standards to internal risk control—empowering staff, modeling safety as a core value, and operating with the goal of managing risks to the “1” in the 1:10:100 Rule instead of the “100”. Always remembering that internal control reduces the need for external influence.
Why is the current focus on forms and rankings problematic?
It drains staff time, fosters burnout, and masks underlying safety issues. It emphasizes process over outcomes, preventing the real kind of progress that can come with a focus on getting it right the first time in the most business-smart, resource-wise, workforce-supportive, defect-free, and patient-focused ways possible.
Why is the “act of chasing more” such a negative when making new money is so important to how a business prospers?
It is not the act of “chasing more” that is the problem. It is how healthcare has chased more since the beginning of its technological revolution. Something that Jim Collins write about in his book titled How the Mighty Fall. It is the undisciplined why that healthcare has chased more with entrenched attitudes that have prioritized scale over quality—quantity over value. Destroying what once allowed healthcare to enjoy tremendous power, influence, earning potential, and goodwill by feeding a slow and insidious story of demise. Always looking for the next silver bullet that will make everything better, blaming the “infamous they” when it doesn’t work out, and never asking what it needs to do different.
What’s the role of leadership in transforming healthcare culture?
Leadership must be the first to change. To prioritize safety and quality outcomes over mere compliance and “chasing more”—setting a clear vision of what it looks like; fostering a culture of transparency and continuous improvement; and walking the talk, not just talking it. Leaders must remember that while the workforce creates the culture, leaders control all the variables that determine what the culture can be. It is leadership’s role to create and manage an environment that ultimately allows for a healthy culture to exist.
What is the 1:10:100 Rule for healthcare?
The 1:10:100 Rule is a basic business principle that speaks to how costs escalate exponentially when, rather than managing risks to the “1” where the goal is the prevention of harm-producing events, risks are managed to the “100”—accruing all the avoidable costs and losses that come with cleaning up messes and dealing with consequences. Spending to some factor of $100, $1,000, $10,000, $100,000, $1,000,000 or more while operating margins shrink. Highlighting the importance of proactive prevention over reactive correction.
What does it mean to manage money and quality like they are two sides of the same coin.
While making money is important for the success of any business, it is how that business manages quality that determines how much money there will be and how earned money gets spent. In any successful business, leaders recognize that making money and managing quality are interdependent and inseparable as it is the quality program that ensures money is spent in business-smart, resource-wise, defect-free, workforce-supportive and customer-focused ways. While how much money is made decides the potential for profitability, how quality is managed to control for avoidable costs and losses decides the ultimate success to be achieved.
How do we start retooling our healthcare environment?
Begin with assessing what drives the negativity in one’s internal culture, reducing unnecessary bureaucracy and getting control of wasteful spending while empowering staff to play a bigger role in managing risks proactively before costly errors can occur. Attending to all the low-hanging fruit that could quickly and easily free up money and manpower.
One-Sentence Summary
Transforming healthcare requires shifting from performative compliance to a proactive safety culture—leading from the front with outcome-driven leadership that empowers staff, creates sustainable control, eliminates waste, and reprioritizes the patient/provider relationship.